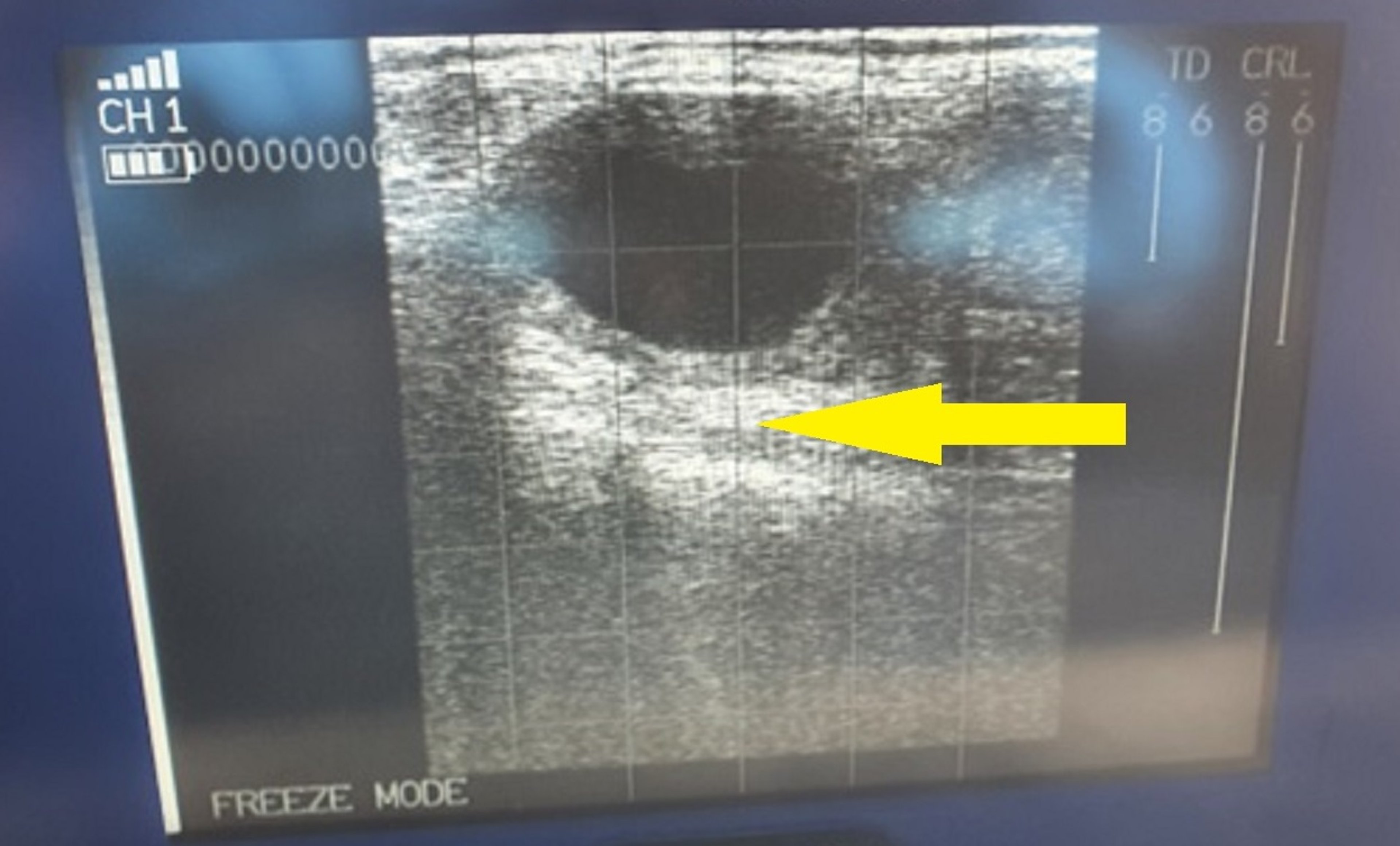
Ultrasonographic image showing a luteal cyst > 30 mm in diameter, with a wall > 3 mm thick (arrow), in the ovary of a cow.
Courtesy of Dr. Jonathan Statham.
Luteal cystic ovary disease is characterized by enlarged ovaries with one or more cysts that have walls thicker than follicular cyst walls because of a lining of luteal tissue. Incidence ratios of follicular versus luteal cysts vary greatly because of differences in the diagnostic skills of individual veterinarians. Typically, luteal cystic ovary disease is defined as the presence of a fluid-filled ovarian structure > 25 mm in diameter, with a wall diameter > 3 mm, persisting > 10 days in the absence of a corpus luteum and usually associated with abnormal reproductive signs. Normal formation of lacunae in the corpus luteum may be incorrectly classified as luteal cystic ovary disease.
Etiology and Pathogenesis of Luteal Cystic Ovary Disease
The basic causes of true luteal cysts are believed to be the same as for follicular cysts. The release of luteinizing hormone may be somewhat greater than that occurring when follicular cysts develop, and it may be sufficient to initiate luteinization of follicles but inadequate to trigger ovulation. Luteal cysts may be an extension of follicular cysts such that the nonovulatory follicle is partially luteinized spontaneously or in response to hormonal therapy.
Clinical Findings of Luteal Cystic Ovary Disease
Luteal cysts are accompanied by normal conformation and anestrous behavior. Rectal palpation reveals a quiescent uterus characteristic of the luteal phase of the estrous cycle. Luteal cysts are recognized as smooth, fluctuant domes protruding above the surface of the ovary. Usually they are single structures.
Luteal cysts are differentiated from follicular cysts on the basis of palpable characteristics of both their structure and the uterus and, to some extent, on the basis of the cow’s behavior. Progesterone assay and ultrasonographic examination can assist such differentiation; with either method, however, a final diagnostic decision remains somewhat subjective.
On attempts to manually rupture the cystic structure, follicular cysts burst or rupture under minimal pressure while luteal cysts cannot usually be ruptured with reasonable force. Both types of cysts potentially respond to treatment with luteinizing hormone or Gn-RH; however, PGF2alpha will lyse some luteal cysts and generally all diestrous corpus luteum structures.
Treatment and Control of Luteal Cystic Ovary Disease
The preferred treatment for luteal cystic ovary disease is luteolytic doses of PGF2alpha, if a correct diagnosis can be ascertained. Normal estrus is expected in 3–5 days after the start of treatment. The major limitation of this treatment is the difficulty in accurately estimating the amount of luteal tissue present. If the structure being diagnosed as a luteal cyst is actually a developing corpus luteum (sometimes called a cystic corpus luteum; see Cystic Ovary Disease and Cystic Corpus Luteum in Cows), it may not respond, because dairy cows do not become highly responsive to the luteolytic action of PGF2alpha until day 6 after estrus.
Ultrasonographic examination is increasingly common in modern practice and facilitates the diagnosis of ovarian structures. Luteal cysts also respond to the treatment with hCG and Gn-RH that is effective against follicular cysts; however, the next estrus could be delayed as much as 21 days after treatment.
Manual rupture of luteal cysts is not recommended, because of the risk of trauma and hemorrhage. Because estrus detection practices are poor on many dairy farms, the preferred treatment for both follicular and luteal cysts is the administration of intravaginal progesterone/prostaglandin or the Ovsynch fixed-timed artificial insemination protocol. This protocol promotes timely breeding in affected cows after treatment.